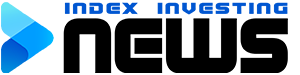© Reuters. Elizabeth Kutschke spends time at the park with her 2-year-old son, Ben, who was diagnosed with spinal muscular atrophy, an inherited disorder which is the leading genetic cause of death in infancy globally and leaves children too weak to walk, talk, swal
2/5
By Deena Beasley
LOS ANGELES (Reuters) – Baby Ben Kutschke was diagnosed at three months with spinal muscular atrophy, a rare inherited disorder which is the leading genetic cause of death in infancy globally. It leaves children too weak to walk, talk, swallow or even breathe.
So when in 2021 his parents heard about Zolgensma – a one-time therapy costing millions of dollars that promises to replace genes needed for the body to control muscles – they had high hopes.
They were disappointed.
After treatment with the $2.25 million therapy at almost eight months old, Ben was able to hold his head up for a few seconds – a significant milestone, his mother Elizabeth Kutschke told Reuters. But he did not advance to rolling over or sitting up, and after a few weeks doctors recommended the family add another drug to help him.
“I just started to worry,” she said from their home in Berwyn, Illinois. “He wasn’t getting worse, but the gradual progress we had seen … was no longer happening.”
Ben is one of a growing number of patients with spinal muscular atrophy (SMA) whose doctors are turning to additional drugs on top of the gene therapy, six top U.S. neurologists told Reuters.
Their experience raises broader questions around other high-cost gene therapies coming to market, sometimes after accelerated regulatory approvals, drug pricing experts said.
Zolgensma, launched in 2019 by Swiss-based healthcare group Novartis as a “potential cure” for SMA, was the most expensive drug in the world at the time.
Gene therapies work by replacing genes – the body’s blueprint for its development. The gene Zolgensma delivers instructs the body to make a protein vital for muscle control.
Other SMA therapies need to be taken continuously, but Zolgensma’s price was justified by hopes this revolutionary approach could beat the condition once and for all.
Zolgensma has been given to more than 3,000 children globally, with 2022 sales of $1.4 billion representing 91% of gene therapy sales worldwide, according to the IQVIA Institute for Human Data Science. In the U.S., where costs are borne by government health programs such as Medicaid as well as private insurance, IQVIA estimated Zolgensma sales totaled $434 million last year.
It has worked well for many. Novartis’ data presented in March shows that depending on the timing of treatment, most patients have gone on to swallow, breathe, or even walk independently, said Sitra Tauscher-Wisniewski, vice president at Novartis Gene Therapies. Some are able to run and climb.
Three of six families interviewed by Reuters whose children received Zolgensma said they were progressing as well as hoped; Ben’s was the only one to turn to another treatment.
But Novartis’ data also shows almost one-third of children in an ongoing study went on to be given other drugs.
If gene therapies do fall short, it becomes harder to justify prices that researchers have argued are already poor value.
“The perception that Zolgensma is going to be a complete cure … is not coming to fruition from the data we have seen over the last four years,” said Dr. Roger Hajjar, director of the Mass General Brigham Gene & Cell Therapy Institute.
“Following the injection of Zolgensma you are basically going from a deadly disease to a more chronic disease state,” he said, adding that many patients would not survive without this treatment.
Novartis said Zolgensma has been “transformative,” but each child’s journey is unique and outcomes can vary. It says there is no evidence additional therapies can help. Notably, it has dropped the term “potentially curative” – common in its analyst calls in 2018 and 2019 – from descriptions of Zolgensma, instead calling it a “one-time treatment.”
“People still have misconceptions about Zolgensma,” Kutschke told Reuters. “It is a treatment, not a cure.”
IN THE PIPELINE
Novartis CEO Vasant Narasimhan spelled out the pricing argument in a 2018 call: “Payers appreciate that when you deliver a potentially curative therapy that takes cost out of their healthcare system and enables people to live, hopefully, a more normal life, they are willing to pay and they see the value,” he said.
The multimillion-dollar pricing strategy is not unique. More recently, the first hemophilia gene therapy approved by the U.S. Food and Drug Administration was priced by CSL (OTC:) Behring at $3.5 million; 26 more gene therapies are in late-stage development, according to IQVIA.
Drugmakers say the long-term benefits are worth it. CSL said it is confident that its treatment can generate cost savings and has offered partial refunds if patients need to resume injections of blood-clotting proteins in the first four years after the therapy.
Novartis offers payment by installments – although it said no one in the U.S. has taken them. It also has plans linking payment to how well a patient responds, but said U.S. refunds under them have been rare.
The economics of treating the relatively small number of patients make a high price tag imperative for manufacturers.
“One of the arguments is you’re saving all of these millions of dollars down the line,” said Stacie Dusetzina, professor of health policy at Nashville’s Vanderbilt University School of Medicine.
“But if you found out later on that oh, actually you have to get most of those other treatments, I think the question is, ‘was that price really a fair price to begin with?'”
The Institute for Clinical and Economic Review (ICER), a drug pricing research group, has said Zolgensma’s maximum price should be $900,000 – less than half its current cost.
The two other available SMA treatments are also not cheap.
Biogen (NASDAQ:)’s Spinraza, injected into the spine, has a U.S. list price of $800,000 in the first year followed by maintenance doses at $400,000 a year. Roche’s Evrysdi, an oral solution, costs $100,000 to $340,000 per year depending on how much the patient weighs.
Both Biogen and Roche said studies of their drugs as treatments for patients who do not respond sufficiently to Zolgensma have been encouraging so far. Biogen’s Chief Medical Officer Maha Radhakrishnan said a second drug could still add value given the high cost of caring for severely disabled patients.
The fact that some children need treatment with other expensive drugs after Zolgensma shows that the gene therapy represents “poor value,” said Steven Pearson, ICER president.
It’s a headache for health insurers, who usually cover the full cost of Zolgensma upfront: It’s not yet clear how to manage a payment plan over time, and that would require more real-world data on how patients respond, said Sree Chaguturu, chief medical officer at CVS Health (NYSE:), which owns health insurer Aetna.
“How long do you actually need to monitor and track those patients?” he said, noting that Americans commonly move between different insurance plans.
“DOING AMAZING”
Many parents of children with SMA say Zolgensma is worth it.
Amanda Cook, a 32-year-old bookkeeper in Lebanon, Virginia, already knew when she gave birth to her son Weston in 2021 that he was diagnosed with SMA: It had led to the death of his older brother, Jackson, at 7 months.
Weston had a flaw in the gene that produces a protein critical to the function of cells that move muscles. The lack of that protein, known as SMN (survival motor neuron), results in SMA, which affects fewer than 300 babies a year in the United States.
But he had Zolgensma at 11 days old and “is ahead of everything, honestly,” Cook said.
All therapies have been stopped and he is “doing amazing as a true 2-year old.”
The treatment works best when infused as soon as possible after birth – some patients can begin to suffer from degeneration before birth – and Ben Kutschke was a relative latecomer.
His parents saw him having problems when he was about a month old. Formula spilled from the corners of his mouth. He couldn’t hold a pacifier; his doctor suggested they try different sizes but it became clear his condition was serious when Elizabeth heard liquid slipping down his windpipe.
Ben was found, like about 60% of cases, to have the most severe form of SMA which often leads to paralysis and death before age two.
“The earlier and better preserved the nerves are, the more likely you are to have success,” said Dr. Jerry Mendell, director of the gene therapy center at Nationwide Children’s Hospital in Columbus, Ohio and principal investigator in the Zolgensma trials.
Zolgensma is becoming available to younger babies across the U.S.: Most states screen newborns for it, and health insurers typically cover Zolgensma for children with the most severe form.
ANTIBODIES
But even after diagnosis, not all children are immediate candidates.
Zolgensma delivers the gene through a modified virus. Ben had already been exposed to the virus in nature and had developed antibodies, which would neutralize the replacement genes in his body.
Dr. Russell Butterfield, pediatric neurologist, University of Utah Health and Intermountain Primary Children’s Hospital, said it’s “not all that rare” for babies to have antibodies to the vector. He put the incidence at 15% to 20%.
Babies can also be ineligible due to issues such as liver problems – Zolgensma’s label warns it can cause these. Last year, two children in Russia and Kazakhstan died of acute liver failure several weeks after receiving it.
Ben was originally treated with Evrysdi, which aims to boost SMN levels directly. It took months for his antibody levels to fall to the point he could start Zolgensma.
“When they did say the antibodies were down, oh I cried on that phone call,” Kutschke said.
When he finally received Zolgensma, Ben’s hand movements became smoother and he was able to lift his head, “but then after that big rocket forward in progress, it seemed to just stall out,” his mother said.
The body develops antibodies to the virus used, so each therapy using it can only be administered once. Doctors recommended a third treatment, Biogen’s Spinraza.
“REAL LIFE”
The most recent Novartis data, updated in March, shows this was not unusual. Its study found that 24 of 81 children given Zolgensma as of May 2022 had been subsequently treated with other SMA drugs. Novartis declined to provide details on them.
“There are a whole lot of things that happen in real life circumstances” to affect the utility of treatment with Zolgensma, Mendell said. For less responsive patients, Mendell said it is reasonable to use other treatments.
But it can be difficult to get insurance coverage after Zolgensma. Some health plans explicitly exclude add-on therapies if a child received it, according to policies posted on their websites.
Kutschke said her insurance company UMR, part of UnitedHealth Group (NYSE:), balked at reimbursing another drug. A spokesperson for UnitedHealth declined to comment.
Kutschke said UMR reasoned that Ben “should be fine” after getting Zolgensma – “Which is really heartbreaking because we thought he would be too.”
It took nearly six months of paperwork and appeals – supported by Ben’s medical team – before payment for Spinraza was approved.
Since then Ben, who now uses a wheelchair at age 2, began talking a lot more. He was suddenly able to move his lower body, his mother said.